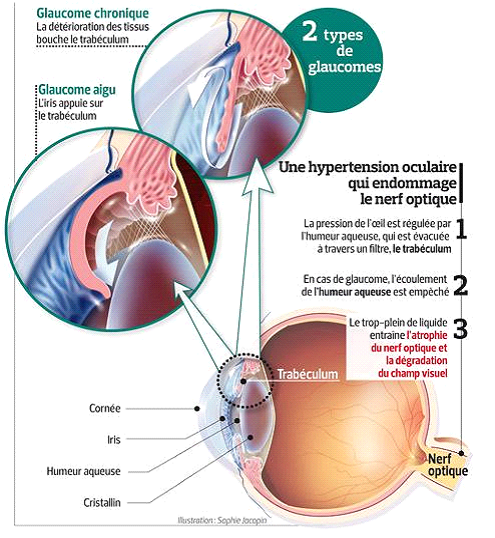
What is glaucoma?
Glaucoma is an irreversible damage to the optic nerve and high pressure in the eyes is a strong risk factor. Rarely, glaucoma can also occur with normal eye pressure.
Damage to the optic nerve
leads to loss of the peripheral field of vision and, in severe cases, can lead to loss of central vision as well.
Glaucoma cannot be cured, but if detected early enough, it can be stabilized to preserve
sight.
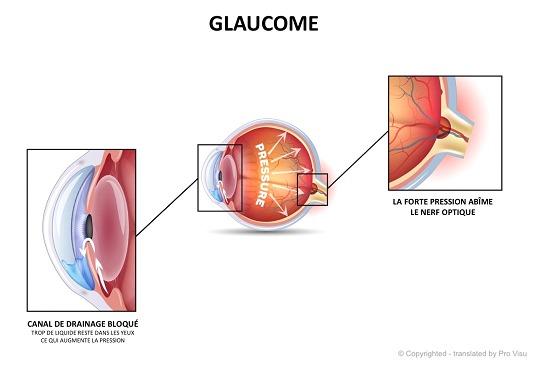
How does glaucoma develop?
Inside the eye, a liquid called aqueous humor is continuously secreted by the ciliary body. This fluid circulates in the anterior part of the eye to bring the necessary nutrients to the tissues. The
aqueous humor passes through the space between the lens and the iris, through the pupil and arrives in the anterior chamber of the eye, from where it is drained by the trabecular meshwork. Trabecular meshwork is a natural
drain that releases the fluid into a channel that, in turn, releases it into the blood stream on the outer surface of the eye. Anything that can block this normal circulation causes an increase in pressure. Increased
pressure in the eye leads to compression of the optic nerve, which conveys visual information to the brain. The destruction of optic nerve fibers is irreversible and results in a permanent loss of visual field that can lead
to blindness.
Who are the people most at risk for glaucoma?
Glaucoma can affect anyone at any age but it is more frequent in people with the following risk factors:
⦁ Age of 40 and above
⦁ Family history
of glaucoma
⦁ Hypermetropia
⦁ Diabetes
⦁ African descent
How to diagnose glaucoma?
In order to diagnose glaucoma, three tests are necessary:
⦁ Measurement of intraocular pressure
⦁ Examination of
the optic nerve head. The optic nerve head contains nerve fibers that arrive in the eye and is the portion of the optic nerve that your ophthalmologist can examine at the bottom of the eye. If the optic nerve head is
suspicious, your ophthalmologist will provide you with more accurate optic nerve exams such as an optical coherence tomography (OCT), a very accurate imaging that allows you to assess and track optic nerve damage.
⦁ Examination
of the visual field. The visual field exam can help to determine the extent of vision damage caused by glaucoma.
What are the different types of glaucoma?
Chronic glaucoma:
Chronic glaucoma is by far
the most common type. It is caused by a progressive obstruction of the trabecular meshwork, the natural drainage system of the eye, resulting in an increase in eye pressure. Chronic glaucoma is often described as a "silent
thief" of vision. When glaucoma is not detected early or not managed appropriately, it can result in a slow, progressive, and painless vision loss, which in the most severe cases can lead to blindness. People with chronic
glaucoma do not notice anything until their glaucoma is advanced. Appropriate treatment and follow-up help to stabilize the patient’s vision.
Chronic glaucoma is usually classified into two broad categories:
⦁ In primary
glaucoma, the eye’s natural drain, trabecular meshwork, works less well without any obvious cause, resulting in increased pressure in the eye.
⦁ In secondary glaucoma, certain diseases, medications, trauma or eye surgery, eye
inflammations, and some other factors can lead to drain dysfunction. This damage to trabecular meshwork results in increased pressure in the eye. In this type of glaucoma, it is useful to treat the identified cause where
possible.
The treatments available for chronic glaucoma are as follows:
⦁ Medical treatment: It consists of eye drops or tablets and is intended to decrease the production of aqueous humor or increase the drainage of the
eye.
⦁ Laser treatment: Laser trabeculoplasty targets trabecular meshwork directly to increase filtration. With good results, the effects of this intervention can sometimes be short-lasting.
⦁ Surgical treatment: If
the medical treatment and laser are not effective or if the side effects are too great, surgery may be necessary. Surgery is designed to reduce intraocular pressure. Your surgeon will choose the most appropriate procedure. Refer
to the surgical portion of glaucoma on our website for more information.
Acute glaucoma:
Acute glaucoma is a sudden increase in eye pressure due to a blockage of the circulation of aqueous mood by the iris. The
space between the lens and the iris through which the aqueous humor must flow is abnormally narrow. The aqueous humor then accumulates behind the iris and causes it to bulge forward, amplifying the fluid retention process. In
some cases, peripheral iris may block the liquid outlet. The result of this blockage is an immediate and significant increase in the eye pressure, causing severe unilateral headaches, nausea, red eye, blurred vision and halos. If
not treated quickly, acute glaucoma can cause irreversible damage. Laser surgery is performed to decrease fluid retention by creating a small opening in the iris (laser iridotomy).
A narrow angle is a condition that
puts one at risk for an acute glaucoma attack. This condition, more common in people with hypermetropia, is characterized by an abnormally narrow space between the iris and the cornea. If the angle formed by the iris
and cornea (irido corneal angle) is narrow, laser treatment should be performed to prevent an acute glaucoma attack.